Most common ocular and visual conditions
Click on the item to learn more
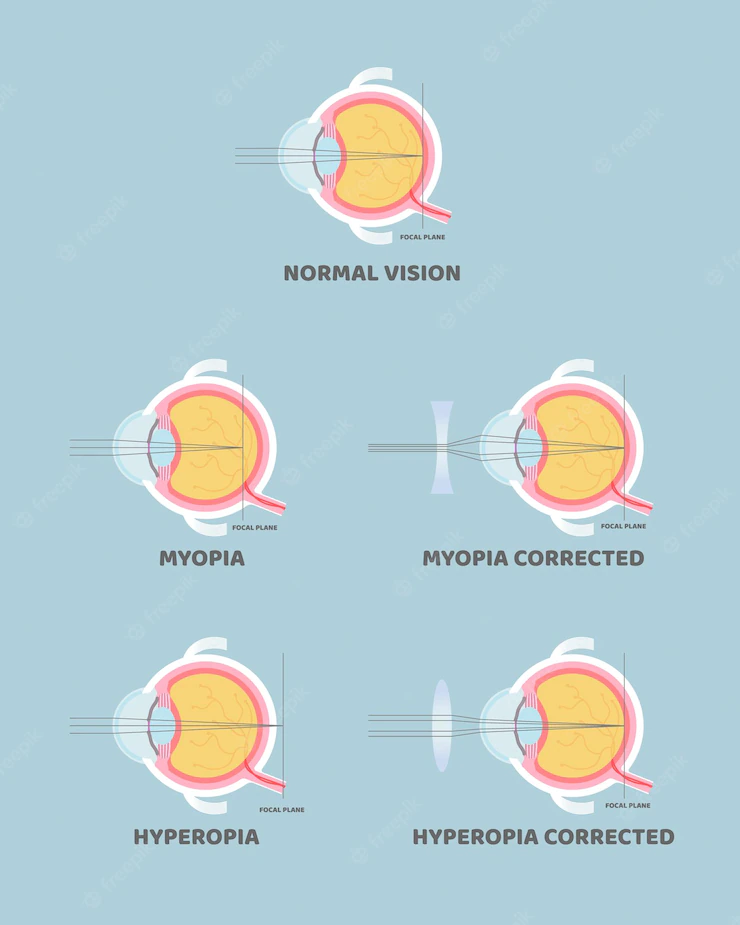
Myopia, Hyperopia, and Astigmatism
These conditions, properly called “refractive errors”, result from an anomaly in the optic system of the eye. In simple terms, hyperopia is when the eye is “too short”, myopia when the eye is “too long”, and astigmatism when the surface of the cornea is irregular. Approximately 50% of the population suffers from at least one of these issues. Depending on the magnitude and certain other considerations, the correction can be achieved by spectacles, contact lenses, or one of many surgical techniques.
Dry Eye
The external surface of the eye is exposed to the air, and there is a liquid coating called “tear film”, which aims to maintain the required moisture levels. For many reasons (air conditioners, long time spent reading or in front of electronic screens, or certain illnesses, for example) this tear film might not function in a perfect way, resulting in very common dryness symptoms such as red eyes, pain, burning sensation, blurry vision, and even paradoxically, excess tearing. Dry eye is a spectrum between “mild”, which leads to complaints about quality of life without significant alteration of vision, to “severe”, where we often observe an important compromise in the ability to independently navigate the world. Treatment usually depends on the causes and severity of the problem.

Blepharitis
The margin of the eyelids, where the eyelashes are born, has the important function of producing and secreting an oil, called meibum, which aids the tear film in lubricating the eye. Sometimes, this oil is generated in an excessive and anomalous manner, resulting in the accumulation of bacteria, and the chronic inflammation of the eyelids (a process analog to acne on the rest of the face). Swelling, wax, red eyes, styes, and other symptoms of dry eyes are extremely common in the general population. The solution starts by a good eyelid hygiene technique.
Droopy eyelid
The small muscles that keep the eyelids up must remain active for many hours each day. When one of them or both start drooping, the causes can be many. They go from very common ones like a normal part of ageing, or allergies, to very rare ones, like neurologic diseases that need immediate treatment. A complete history and ocular examination are typically able to focus the diagnosis process and subsequent treatment.
Conjunctivitis and allergies
The very thin and transparent “skin” that covers the white wall of the eye is called conjunctiva. It contains very narrow blood vessels. When these capillaries dilate and accumulate more blood, the eye turns red. This is called conjunctivitis, and depending on the reason for the inflammation, we can have viral, allergic, bacterial, or toxic conjunctivitis, among some others. History and physical examination are usually sufficient to diagnose and offer treatment.
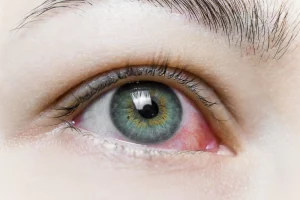
Ptreygium
This very common condition happens when a part of the conjunctiva, or the transparent “skin” that covers the white wall of the eye invades the limits of the cornea and expresses an abnormal growth. It happens, in a few words, due to excessive sun exposure and a chronic irritation on the surface of the eye. Its solution is surgical. Even though in most cases we offer surgery due to cosmetic concerns, in some advanced cases, a prominent pterygium can generate blurry vision or foreign body sensation. Surgery for pterygium excision is a rapid and safe process, although in a small percentage of people, the lesion can recur in the future.
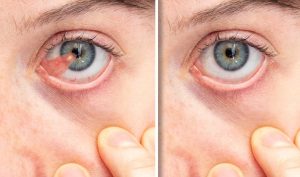
Keratoconus
The frontal layer of the eye, through where the light comes in, is called cornea, and it is a transparent lens. In the majority of cases, this lens has the shape of a soccer ball cut in half (half a sphere), or like an American football cut in half, with two different curvatures (this is called astigmatism). In some people, for several reasons, like eye rubbing, genetics, chronic allergies, among others, an outward bulge is developed in the corneal surface. Think about it like that “bump” that happens when you hit your head. This irregularity on the surface of the lens is felt like blurry vision which, in some cases, worsens over time. This bulging, or ectasia in medical terms, is called keratoconus, and its treatment depends on how early in the process the diagnosis is made. An early diagnosis will usually lead to either observation or to the usage of vitamin B + UV light as a way to strengthen the cornea to prevent worsening, whereas a late diagnosis might entail corneal transplant, either partial, or in some cases, even full thickness.

Corneal erosions and infections
The frontal layer of the eye, or cornea, has an outer coating of cells that regenerate every 3 days, more or less like the skin. If this coating falls off (eye scratches, or in very very dry eyes, for example), the nerves end up exposed and a lot of pain is felt, sometimes also blurry vision. This is called corneal erosion, and even though it sounds serious, it typically closes in less than 3 days. However, during this time, bacteria can become anchored to the cornea and generate severe infections. The treatment consists of the administration of antibiotics and lubrication until the erosion closes.
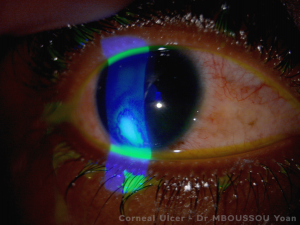
Cataracts
This common condition is not really a disease. A cataract is part of the normal ageing process, like the gradual whitening of the hair. In some people however, for different reasons, like uncontrolled diabetes, or a very bad blow to the eye, they can develop earlier in life. We call a cataract to the opacification (loss of transparency) of the crystalline lens, a structure that we all have inside the eye. As it turns opaque, less and less light reaches the retina and vision is perceived as blurry. Cataract formation is a slow and progressive process, and some people with more strict visual needs (like bus drivers or librarians, for example) might detect them sooner. When the vision is blurry enough to interfere with daily activities and quality of life, the cataracts can be removed with a relatively simple 20-minute intervention called cataract surgery. In the great majority of cases, vision is restored completely.
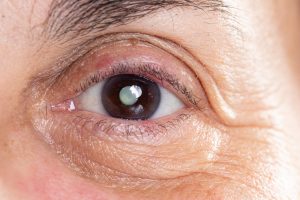
Intraocular inflammation
Underneath the white wall of the eye, there is a layer of blood vessels called uvea. For many reasons, both external (like trauma) and internal (certain autoimmune diseases like lupus or rheumatoid arthritis), these vessels can become inflamed and create negative effects both on the eye and on the vision. Although finding the cause of the uveal inflammation can sometimes be a long and winding road, even frustrating, in great many of the cases it can be achieved with as little as an extensive interrogation and a detailed examination in the office.
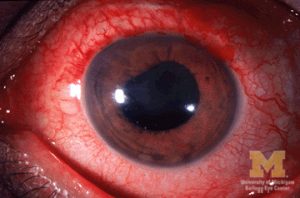
Glaucoma
The eye is like an inflated balloon that has a certain pressure inside. In nearly 5% of the general population, this pressure rises in a silent way, causing permanent damage on the internal walls of the globe and the cable that connects it to the brain. It happens in such a slow way, that usually afflicted patients are not aware of having less vision, until very late in the process. The sensation is not of blurry vision, but more like a slow dimming, like a lightbulb that is progressively extinguished. Glaucoma is one of the most common causes of irreversible blindness. If diagnosed in time, the initial treatment tends to be very simple and the visual decay can be prevented. If found in a latter stage, the objective of the therapy is to arrest or slow down any further worsening. Our best weapon against such a silent illness is a yearly eye examination, preferably with dilation of the pupil.
Ocular Diabetes
The damage done by diabetes to the eyes is responsible for the highest percentage of blindness in the urban areas of North America. Diabetes is a disease in which the blood vessels of the whole body become affected due to the excess glucose (sugar) carried in the blood. The eye has many of these vessels, especially in a place called retina, which is like the film of the camera that takes the actual photo. The more compromised these capillaries become, the less oxygen that reaches this very sensitive part of the eye, which reacts in many different ways, including inflammation, hemorrhages, and the formation of new, fragile blood vessels that can leak or break. The most important factor in the treatment of ocular diabetes is the control of the glucose levels. Additionally, we sometimes make use of combinations of laser or injections as steps that aim to prevent or delay further surgical intervention.
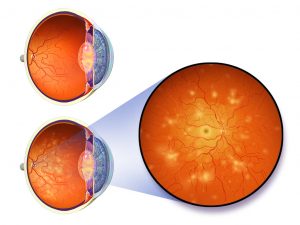
Retinal detachment
The retina is like a wallpaper, adhered to the internal wall of the eye like a film of a camera. On occasions, this wallpaper can become detached and partially hang towards the inside of the eye. The symptoms depend on the degree and size of the detachment. These go from the sensation of new floaters, to a shadow that covers a part of the visual field in one single eye. Early in the process, laser treatment is usually enough to stop the progression, while more advanced detachment typically requires prompt intraocular surgery.
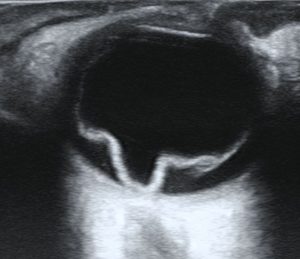
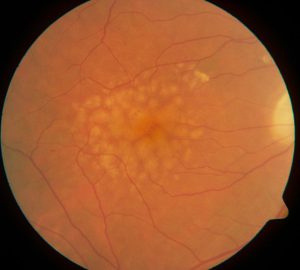
Macular degeneration
Depending on certain genetic or metabolic factors, some people start to accumulate toxic byproducts in their retina as normal ageing progresses. When this accumulation reaches a certain level, the central part of the retina, called macula, suffers changes that end up in its degeneration and the subsequent loss of vision. In the majority of patients, observation and a combination of specific vitamins is all that it takes to monitor the disease. However, some more advanced cases can progress to stages in which we utilize intraocular injections as a method of control.
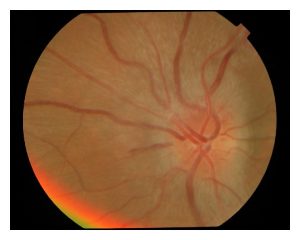
Optic neuritis
The cable that connects the eye to the brain is called “optic nerve”. Due to immunity-related causes, in some people, frequently young women, this nerve becomes inflamed and produces pain on eye movement or alterations in the perception of colors and contrast. Although many of the episodes of optic neuritis are resolved with the passage of time, there is sometimes a relation to some neurologic diseases, in which case timely follow up is desired
Ocular Trauma
Under this term we fit all the effects of an external force on the eye or its neighboring structures. The combinations are virtually infinite and not always immediately symptomatic, which makes it very advisable to have any blow to the eye checked by the ophthalmologist as soon as possible.

